Finding Every Child: How Defaulter Tracking is Re-vitalizing Immunization in Uganda
-
by
AFENET
Finding Every Child: How Defaulter Tracking is Re-vitalizing Immunization in Uganda
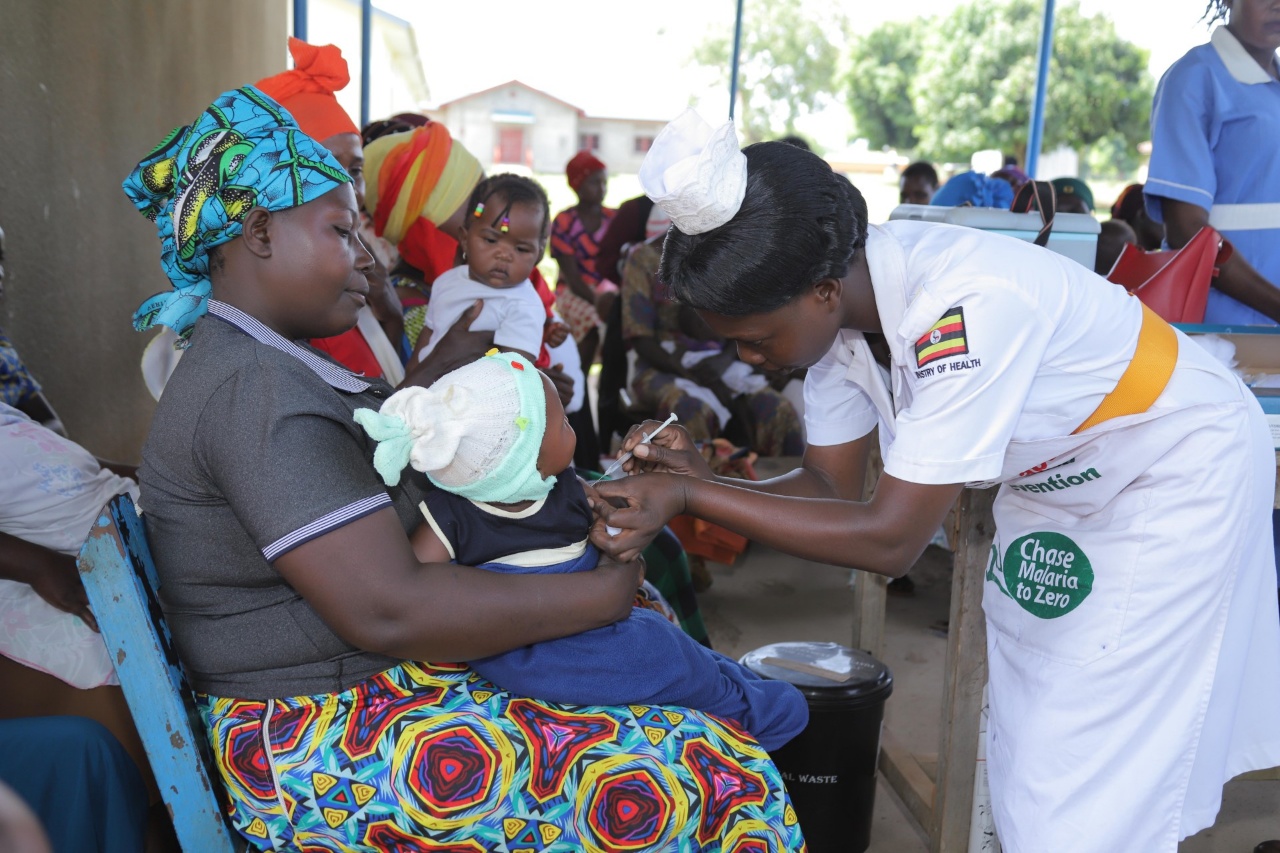
In April 2025, the Uganda Ministry of Health introduced the R21/Matrix-M malaria vaccine into routine immunization—a historic step in a country that remains among the highest contributors to global malaria cases and deaths. Administered at 6, 7, 8, and 18 months, the vaccine offered new hope for protecting young children.
However, early implementation revealed a critical gap. In several districts, first-dose coverage ranged between 20–40%, and thousands of children were missing subsequent doses. Behind every missed appointment was a child at risk. Healthcare workers were not well prepared, immunization registers were incomplete, follow-up systems were weak, and health facilities lacked structured approaches to identify and reach defaulters.
The challenge was clear: vaccine availability alone was not enough. Systems needed strengthening to ensure every eligible child was reached.

From Introduction to Integration
Following the initial rollout in over 100 high-priority districts, challenges emerged: knowledge gaps among healthcare workers, inconsistent data reporting, low demand for the new vaccine, and high dropout rates between doses. In districts such as Busia, Iganga, Luweero, and Butambala, routine immunization systems were strained.
Recognizing that strong systems—not just new vaccines—drive impact, AFENET< with support from the US CDC supported selected districts to fully integrate the malaria vaccine into routine immunization services. The strategy focused on three pillars: capacity building, supportive supervision, and defaulter tracking.
Building Skills, Strengthening Systems
Twenty-two district health team members and 192 healthcare workers received refresher training on immunization schedules, eligibility criteria, and data management. Continuous medical education sessions reached an additional 457 staff. At community level, 1,171 Village Health Team (VHT) members and 159 community health extension workers were mobilized to conduct household follow-ups and mobilize caregivers.
Supportive supervision visits were conducted in 86 health facilities to review child registers, improve data quality, and establish structured follow-up systems.
Defaulter tracking was implemented to identify, line list and conduct community-led home-based follow-up for catchup vaccination on missed vaccine doses.
Turning Data into Action
What the data revealed was sobering. Across the four districts, health facilities identified:
- Over 10,000 children were identified as defaulters in the 4 supported districts. The key vaccines considered were malaria vaccine dose 1, dose 2 and dose 3, as well as measles rubella vaccine dose 1 and 2.
- In many facilities, children had received vaccines that were never recorded. Others were documented as receiving later doses without evidence of earlier ones. Some facilities relied solely on tally sheets, while new antigens were missing from older registers. In several cases, children were vaccinated before reaching the eligible age—highlighting the need for refresher training.
Rather than viewing these numbers as setbacks, districts used them as a starting point for action.
Facilities reorganized registers using a birth cohort system, added columns to capture new antigens, and instituted weekly updates. Children who missed appointments were line-listed and assigned to community health workers for follow-up. Malaria vaccination was integrated into all static and outreach sessions.
Rather than viewing these findings as failures, teams treated them as opportunities. Health workers were guided to register children by month of birth using the cohort system, update missing information weekly, and create additional columns in registers to capture new vaccines. Facilities were encouraged to integrate malaria vaccination into all static sessions and outreach activities.
Most importantly, defaulters were systematically line-listed and assigned for follow-up.
Community Voices: “We Now Know Who to Look For”
In Iganga District, a VHT member shared during a follow-up meeting:
“Before, we waited for mothers to come to the health facility. Now we have names. We know which child missed which dose. When we go to the home, we speak confidently because we have the records.”
In Busia, a facility in-charge reflected on the transformation:
“We realized we had many defaulters, but no plan to follow them. With the defaulter register and support supervision, we are no longer guessing. Every missed child is documented and assigned.”
During mentorship sessions, healthcare workers also expressed renewed confidence. One vaccinator in Luweero noted:
“The CME on EPI schedules helped me understand the timing better. Now I double-check eligibility before vaccination, and I update the register immediately.”
These voices echo a shift from reactive service delivery to proactive child-centered care.
Early Signs of Progress
Since introduction in April 2025, Uganda has achieved coverage of 80% for MV1, increasing from 54% in May 2025.
Supported ddistricts report improved reporting rates and stronger follow-up systems. Health facilities are conducting more static and outreach sessions in poorly performing areas. Routine review meetings are being revitalized, with immunization data guiding local decision-making.
Defaulter tracking has also strengthened broader routine immunization. By identifying children who missed malaria vaccines, facilities simultaneously recovered those who had missed measles-rubella and other antigens—maximizing each contact with the health system.
- 28% (3,100) children have been vaccinated after follow-up by the VHT
- 13 % (1408) children
- 12% (1373) children have migrated to other districts
- For the first time, facilities moved from passive service delivery to proactive child tracking.
Lessons for the Future
The experience underscores several key lessons:
- New vaccines must be accompanied by strong data systems and frontline mentorship.
- Community health workers are essential for closing immunization gaps.
- Regular supportive supervision builds accountability and confidence.
- Prompt facilitation and logistical support for VHTs sustain morale and performance.
As Uganda advances toward its malaria elimination goals for 2030, defaulter tracking is proving to be more than a corrective measure—it is a strategy for equity. By combining accurate data, trained health workers, and empowered communities, districts are ensuring that no child is left behind.